
Eye Health - Hadleigh, Essex
We know that your eyesight is incredibly precious to you. When you intrust us with your health we take that responsibility very seriously indeed.
Forbes Opticians provides a range of examinations to keep your eyes healthy. Please choose from the links below to find more information.
Headaches

We are always happy to examine patients suffering from headaches to rule out an ocular cause.
Symptoms and history are very important when trying to establish the cause ofheadaches so we will need to know:
- How long you have had them for?
- How often they occur and at what time of day?
- Is there any pattern?
- Where on the head does it ache?
- What makes it better and whatmakes it worse?
- Are there any associated symptoms such as nausea or visual disturbances?
If headaches appear to be associated with specific visual tasks such as computer work, reading or driving we will investigate how well the eyes focus for these tasks and if the eyes work well together as a team. If a problem is found it can generally be resolved with appropriate spectacles.
However if headaches do not seem to have an ocular cause we are able to check some relevant aspects of eye health and visual function and the refer you on to your GP with this information for further investigation.
The best advice with headaches is to be sensible; you know better than anyone what type and frequency of headaches are normal for you.
Any significant change in your headaches should be investigated.
Glaucoma
Glaucoma is the second most common cause of blind registration in the UK. The condition involves damage to the optic nerve caused by raised pressure in the eye.
Open angle glaucoma
The eye is full of fluid called aqueous. The aqueous is constantly being produced within the eye and drained out of the eye. It is the balanc between the production and drainage of aqueous that determines eye pressure. In glaucoma too much is made and not enough is drained, pressure increases and the optic nerve is slowly damaged.
Optic nerve damage in glaucoma results in loss of side vision and if untreated can progress until all vision is lost.
If you are at risk of glaucoma regular screening and early diagnosis is very important.
Who is at risk
Glaucoma can affect anyone but certain groups are more at risk than others. These include:
- People over 60 years of age
- People who have a parent or sibling with glaucoma
- People with myopia
- People of African or Black Caribbean heritage.
You can also be at risk if, on examination, you have been found to have:
- Suspicious optic nerve cupping
- Higher than average intra-ocular pressure
- Thin corneas
- Narrow anterior chamber angles.
How we screen for glaucoma
Glaucoma is a condition of the optic nerve so initially we need to check the optic nerves for any evidence of damage.
Normal optic nerves have a pink rim made up of healthy nerve fibres and a pale centre where nerve fibres are absent called the cup. In glaucoma nerve fibres die and over time the cup gets bigger and the rim gets smaller.
Checking the pressure of the eye is also very important, but so is measuring corneal thickness. If the cornea is thin we tend to underestimat the pressure and also eyes with thin corneas tend to copeless well with higher pressures. Ideally then, we need to know the pressure of the eye and the corneal thickness.
If there is damage to the optic nerve caused by pressure there may also be side vision loss so it is important to check the field of view.
Subtle changes in cupping are incredibly difficult to detect and, in our opinion, the best way is utilising progression analysis software. For this we now use the latest Zeiss Cirrus OCT.
This piece of equipment uses very high-resolution ultrasound to measure the parameters of the optic nerve and analyse change over time. The OCT allows us to detect early nerve fibre loss with confidence.
Treatment
If you are diagnosed with glaucoma the most common treatment is eye drops that reduce aqueous production and increase drainage resulting in a lowering of the eye pressure. However the earlier the diagnosis the better the prognosis will be.
Closed angle or acute glaucoma
Aqueous leaves the eye through the drainage angle. Very narrow angles can restrict outflow, raising the pressure and if the angle closes completely the pressure can get very high very quickly resulting in an extremely painful eye. This is called acute glaucoma. It is an emergency and needs immediate treatment by a specialist.
Luckily acute glaucoma is rare (less than 10% of all glaucoma) and often can be avoided. We try to prevent emergences like this by routinely ultra-sounding narrow looking angles so those most at risk can be identified and preemptive action taken to prevent closure in the future.
If you are concerned about glaucoma and would like to be assessed, call us on 01702 555 345 for an appointment.
Age Related Macular Degeneration
Age related macular degeneration (ARMD) is the largest single cause of blindness in the UK. The macular is the very centre of the retina and macular damage results in loss of central vision causing great difficulty with tasks such as reading.
It is believed that ARMD is caused by damage to the macular over time by short wavelength blue light combined with free radical damage.
This is much the same process as sunshine causing skin damage and just as some of us are more at risk of sun burn some people run a higher risk of ARMD.
Risk factors for ARMD
Risk factors for ARMD include:
- Having a close family member with the condition
- Smoking
- A diet high in fat and cholesterol and low in antioxidant-containing fruit and vegetables
- Age – the older you are the higher the risk
- High levels of sun exposure
- Hypertension
- Obesity
- Having blue eyes and fair skin.
Early ARMD
In early ARMD the vision is normal, but when the macular is carefully examined there are changes in the macular pigment and/or yellow sub-retinal deposits called drusen.
Late or visually consequential ARMD
If these retinal changes are advanced enough the vision can be affected. This can happen in two ways:
- The macular may slowly ‘wear away’, becoming thinner until areas of central retina are absent. This is dry age related macular degeneration.
- In some cases blood vessels leak into the macular causing sudden blurring and distortion of the vision. This is wet age related macular degeneration.
It is worth noting that dry ARMD can become wet ARMD at any time. All it takes is for a blood vessel to leak for the classification to change.
How ARMD is treated
There is no effective treatment for dry ARMD but there is growing evidence that a diet rich in antioxidants (particularly macular pigments) may reduce the risk of progression.
Wet ARMD can be treated but needs to be caught early. The earliest sign of a blood vessel leaking at the macular is distortion of central vision. Anyone noticing distortion needs to attend the practice that day so that we can confirm the diagnosis, ideally with an OCT examination, and take the appropriate action.
Macular pigment
The macular contains a yellow pigment that acts like ‘sun screen’ protecting the macular from the damaging effects of short wavelength blue light and neutralising free radicals in the same way that sun screen protects the skin from burning and premature ageing. Low levels of macular pigment increase the risk of ARMD.
If you have a close relative with macular degeneration then you should consider eating more vegetables that are naturally rich in macular pigments as well as taking sensible precautions to reduce risk such as not smoking and wearing sunglasses in bright conditions.
If during an eye examination you are found to have significant macular changes that put you at risk of visual impairment then you may wish to take a macular pigment supplement. Also individuals with sight loss in one eye due to ARMD are advised to take a supplement to reduce the risk of sight loss in the second eye.
OCT – the perfect tool for screening OCT (Ocular Coherence Tomography) is a truly amazing diagnostic tool. It allows us to find wet macular changes when symptoms are minimal and no problem is apparent with conventional equipment. The OCT uses ultrasound to look inside the macular in minute detail so that the tiniest changes become obvious. Early diagnosis means early treatment and early treatment means better outcomes.
Macular pigment diet supplements
Studies have shown that supplementing a normal diet with high levels of macular pigment in tablet form will generally result in a significant increase in macular pigment levels in the eye. This ‘building’ of macular pigment usually takes about three months and treatment must be continued to maintain optimal levels.
Long-term studies will be required before we can say for certain that increasing macular pigment levels definitely reduces the risk of sight loss due to ARMD but there is growing evidence that this will be the case.
If you are concerned about ARMD and would like to be assessed, call us on 01702 555 345 for an appointment.
Floaters & Flashes

Sudden onset floaters and flashing lights are one of the most common symptoms that present to our optometrists.
Floaters are often described to us as looking like ‘grey spots’, ‘tadpoles’ ‘broken rings or ‘cobwebs’ in the vision that move away as the eye moves towards them. They are often associated with flashes of light in the side vision.
These symptoms are common and are caused by a natural process in the eye that involves the vitreous jelly that fills the eye peeling away from the retina. This ‘rearrangement’ of the jelly is called a posterior vitreous detachment (PVD) and is quite normal. The jelly takes about five weeks to peel away completely and during this process floaters and occasional flashes are normal.
Complications
However things do not always go smoothly. In about five percent of people the vitreous becomes ‘snagged’ on a piece of retina as it peels away, so that as the eye moves the weight of the vitreous is pulling on one small piece of retina. This can result in a retinal tear.
Retinal tears are a real concern as if they are not treated quickly they can progress to a retinal detachment which is much more serious. Detachments are emergences and need to be seen by an eye specialist immediately so that the retina can be reattached and the sight can be saved.
What you should do if you notice floaters or flashes
Anyone with sudden onset floaters and flashes needs to be examined by an optometrist immediately to check for retinal holes or tears. Even if the eye is fine it should be checked again after about five weeks, when the jelly has peeled away completely, to make sure that no tears have formed during the process of peeling. During this time you can monitor your own eyes, looking out for symptoms that may suggest a tear or detachment.
These symptoms include:
- A sudden increase in floaters – often more than you can count
- The flashing lights increasing in intensity over time rather than decreasing
- Shadows in the vision or grey areas where vision is lost.
We expect the symptoms to get better over time so any sudden increase in symptoms is a concern and needs to be investigated immediately.
What do we do if we find a retinal tear?
Tears in the retina need to be treated straight away to stop them progressing to a detachment. Luckily tears are very easy to treat. A laser is used to make small burns in the retina all the way around the tear. The burn forms a scar and the scar ‘welds’ the retina down so that it cannot detach. This whole procedure is quick, simple and painless.
Remember, if you notice sudden onset floaters, flashes or both you need to be seen straight away. Only a minority of people will have retinal complications but for those who do, early treatment is essential.
Diabetes & The Eye
Diabetes is a condition that can cause eye problems so regular, high quality eye care should be a priority for any diabetic.
Luckily there is an NHS national eyescreening program in place, and we recommend that all diabetics take advantage of this. However this should be complimented by a yearly eye examination by an optometrist.
We suggest that ideally all diabetics are examined with drops in the eyes to dilate the pupils. This allows for a better view of the retina and helps the optometrist to find any retinal abnormalities such as leaky blood vessels. This can also be complimented with a high-resolution retinal photograph to help identify any subtle changes in the central retina and an OCT scan to assess their significance.

Treatment
Diabetic eye problems are treated with great success with a laser. The laser can be used to seal leaky blood vessels and destroy retinal abnormalities such as new vessels.
To reduce your chances of eye problems try to:
- Have regular NHS eye screenings (your GP can arrange these)
- Have a regular eye examination with dilated pupils (do not drive to your eye examination as you cannot drive after drops).
Also make sure that you:
- Maintain good blood sugar control
- Control blood pressure
- Take regular exercise
- Eat a healthy diet
- Do not smoke.
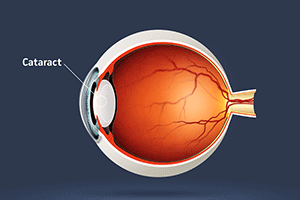
Cataract
The eye has a natural lens situated just behind the iris (the colored part of the eye). When we are young the lens is completely clear but as we age the lens yellows and develops opacities. If these changes are significant we call it cataract.
Cataract can be considered a normal ageing change and is found in 60% of people over 60 years of age and virtually everyone over 70.
Most people with early cataract are symptom free, but if the cataract develops significantly the symptoms include:
- Blurring of distance vision
- Difficulty reading, especially in low ligh
- Glare, especially when night driving or with low sun.
If a patient has a debilitating amount of cataract it can be removed. However what one individual finds debilitating another may find quite acceptable, depending on their circumstances. For example, a computer worker who regularly drives at night may feel debilitated with less cataract than a retired non-driver.
Treatment
Cataract surgery is a very low risk procedure that involves removing the eyes natural lens and replacing it with an artificial lens. The surgeons are very highly skilled and can complete the surgery in about 10 minutes under local anaesthetic.
If surgery is required in both eyes the worst eye is operated on first and then the second, when the first is fully recovered.
You will need to come for a sight test about five weeks after surgery as the spectacle lenses will need to be changed at this time so that you can fully appreciate the improvement in your vision.
Dry Eye
Dry eye is one of the most common and debilitating conditions seen at our practice.
The symptoms of dry eye include:
- Feelings of dryness, grittiness or soreness, which get worse throughout the day
- Intermittent blurring of the vision
- Redness of the eyes
- Watering eyes, particularly when exposed to wind
- Eyelids that stick to the eye when you wake up.
There are two underlying causes for dry eye problems.
Not enough tears are made
This is generally caused by problems with the lacrimal glands that produce the tears and can be associated with conditions such as Sjogrens syndrome.
Plenty of tears are made but they evaporate too quickly
This type of dry eye is associated with eyelid problems such as blepharitis, which often results in dysfunction of the oil producing glands. The purpose of oil is to sit on top of the tear film and slow evaporation. Not enough oil results in fast tear evaporation and dry eye symptoms.
Treatment
We need to know the cause of dry eye so that the appropriate action can be taken to increase the amount of tears in the eyes and/or to slow down the evaporation so they stay in the eyes for longer.
Our optometrists have an interest in dry eye diagnosis and treatment and would be happy to examine your eyes if you feel you may be suffering from this very common problem. Call us on 01702 555 345 for an appointment.
Blepharitis
Blepharitis is a condition where the rims of the eyelids become inflamed. This can result in symptoms such as burning, soreness or stinging of the eyes, crusty eyelashes and itchy eyelids.
Blepharitis is often caused by a bacterial infection of the lids but can also be associated with other conditions such as seborrhoeic dermatitis (the same condition that causes dandruff) and rosacea (a skin condition that causes red blotches on the face)
There are no serious complications of blepharitis but sufferers have an increased risk of:
- Dry eye
- Lid cysts
- Styes
- Conjunctivitis.
Treatment
Blepharitis cannot be cured but regular lid cleaning will greatly reduce the population of bacteria on the eyelids, which results in less symptoms and complications.
We stock a variety of cleaning solutions specifically designed to treat this condition that are highly effective but also kind to the eyes. But remember, the lids should be cleaned every day whether you have symptoms or not.
Visit our Eyelid Care Website for more information.
